My High-Risk Pregnancy Success Story
Hi there! I’m Christina, a mom of two littles, a licensed mental health therapist, and a soon-to-be children’s book author! Thanks for checking out my site. Look around! I’m sure there’s something here for you! Read on to learn more about my high-risk pregnancy success story with a bicornuate uterus.
How my pregnancy was labeled high-risk: Finding out about my bicornuate uterus
If you’ve stumbled upon this post, it’s likely that you want to hear good news about a high-risk pregnancy. Well, you’re in the right place.
Back in 2012, when my now husband and I were just dating, I was shocked to find out that my body may not be able to bear children.
I was devastated.
Ever since I was a young girl, I knew I wanted to be a mom. And now, I was learning that it might not be possible because I have what is called a bicornuate uterus.
The bad news was I didn’t know if I would be able to get pregnant, and if I was able to, how would I face the hefty list of risks a woman with a bicornuate uterus may encounter.
The silver lining was that I found out about my anatomical anomaly before ever trying to conceive, so by the time my husband and I were ready to try to grow our family, we knew to be prepared for what might be a tough road.
*Spoiler alert, I successfully carried both my children two years apart to full-term, with one having been in my left horn and one having been in my right. Read my birth stories here!
What is a Bicornuate or Heart-Shaped Uterus?
Put simply, it means a woman’s uterus, which should look like the classic upside pear shape is shaped differently.
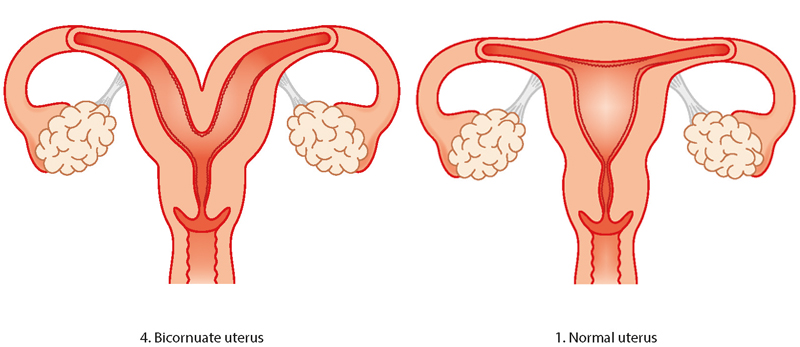
The range of what is known as a Mullerian Duct Abnormality is quite broad.
This could mean that there is a wall, or a septum, going down the center of the uterus, creating two cavities.
Or it could mean that the two sides of the uterus did not fuse correctly when the woman herself was an embryo, leaving the entire uterus pinched in the middle, thus forming two “horns”, or a “heart-shape”. (This is the kind I have. I have two half uteri but they both attach to the same cervix. See image above.)
In some women, they may only have one half uterus. Others have two half uteri, and two cervixes.
In other women, they may even have two vaginas.
A quick Google search will show the various types of malformations. You will also learn about the supposed rareness of this abnormality and the scary risks associated with it.
Before you go down the Google rabbit hole, stop. I already did that for myself, and for you, when I found out my diagnosis. What you will read from website to website is not pretty, and quite deflating.
Here I will share with you the high level risks without going into all the potentialities you might find elsewhere. This is pretty much all you need to know until you speak with your doctor about your specific risks and pregnancy path.
Information about and risks of a high-risk pregnancy with bicornuate uterus:
- A bicornuate uterus is considered very rare, which makes you feel the opposite of lucky. It can feel like you’re the only one with this, but you’re not! Once I started talking to others, I found that at least three other women in my friends, family, and work circles have been diagnosed with the same condition.
- Depending on the severity of the malformation, many women who do have a bicornuate uterus may never even know. If these women have a typical pregnancy and vaginal birth, they may never find out. Many women, if they do find out, do so during a c-section when the doctor is able to see the shape of the uterus.
- Depending on the type of bicorunate uterus you have, the risks are more or less. In general the risks are:
- The egg may not have viable uterine lining and tissue in which to implant, leading to trouble getting pregnant.
- If pregnancy is achieved, the uterine tissue may not behave how it is supposed to in order to provide a good environment for the growing embryo or fetus, meaning a higher risk of miscarriage.
- Then if the pregnancy is sustained, a premature birth or a baby that is not growing as they should be is more likely because the uterus may not stretch to the necessary capacity.
- Finally, if the pregnancy makes it to term, a c-section is likely because there is often not enough room for the baby to flip head-down.
- You will likely be encouraged to be cared for by a perinatal specialist with expertise in your type of uterine condition during your pregnancy. (We actually really enjoyed the extra care and the extra scans to get to see our little peanut at every appointment!)

A High-Risk Pregnancy with Bicornuate Uterus Success Story
Pregnancy is anxiety-provoking as it is, but to go through it with a known condition that may contribute to problems and complications takes it to a whole other level.
My hope is that by reading my success story, you can feel some sense of relief that it is possible to have a successful pregnancy and birthing experience, even though you are high-risk.
I had found a lot of negatives online when I aimed to learn more about my condition. I did not come across one high-risk pregnancy with bicornuate uterus success story which inspired me to write this positive outcome post for you here!
Conception:
We were able to conceive our daughter after just four months of trying, which is within the range of typical! We did not experience a delay in conception due to my uterus shape.
Pregnancy:
We found out at our first scan at 8 weeks that our daughter was in my LEFT horn. She claimed that space and made it her own.
We were very lucky to not have any miscarriages in our family-growing journey.
Aesthetically, I worried that my stomach would be lopsided, or firm on one side and jiggly on the other as the baby grew. Fortunately, baby and belly centered themselves in my torso as our daughter got bigger! My belly looked pretty normal!
We were assigned to a Perinatal Specialist through our hospital system (if you’re in San Diego, you will likely be sent here) which ended up meaning several things:
- Our doctor knew loads about bicornuate uteri. She was fabulous, and because she knew the risks inside and out, and was comfortable with them, she emitted a sense of calm and confidence in my body doing what it needed to do.
- We did have to drive further to our appointments, which was a little tough to manage because my husband came with me to each one (meaning he and I had to take off work more often).
- We got to see our baby a whole lot! The perinatal specialists have some fancy machines and they use them to make sure everything is going well. My belly was not measured by paper tape once because they’d use their tech to measure my baby in utero instead!
- They are sensitive to signs of distress, which could be reassuring that they are on it, or disconcerting that they may find more things to worry about.
- Our medical bills were more expensive than the typical pregnancy’s expenses would be. All those beautiful scans (and the amazing doctor’s skill, experience, and expertise) meant a good bit more money.
During our first pregnancy with my daughter, there was concern that I had Placenta Previa. Spoiler alert: It resolved itself within a couple months!
Besides the special care and concern we received at our appointments, my pregnancy was very normal.
I had morning sickness from week 6 through week 14, I felt better in the second trimester, and I still felt pretty good in the third!
I felt the baby kicking starting at around 18 weeks, which is a pretty normal time to feel movement — even with an anterior placenta.
When I was five months pregnant, my husband and I traveled (with our doctor’s approval) 9,000 miles to attend the wedding of two of our friends in Malaysia! (PS Japan Airlines treats pregnant passengers like royalty.)
I was fearful of premature labor from 24 weeks onward simply because I knew the risk, but I had zero signs of any prematurity. I didn’t even feel any Braxton Hicks contractions!
Labor:
At 40 weeks on the dot (note: not premature AT ALL!), my water broke, I naturally started contracting, and we went to the hospital, where I labored for 12.5 hours (short for first-time births!) before vaginally delivering our beautiful baby girl!
Success!
My experience of pregnancy and birth was very similar with our second child as well!
This pregnancy, our son was in my RIGHT horn, so we weren’t sure if it would comply as well as my left one had with our daughter, but by this time I simply trusted that it would.
I trusted it so much in fact that we chose to not see a high-risk specialist this time, even though the pregnancy was still technically high-risk.
We saw the OB at our local hospital, we only had two scans (to confirm pregnancy, and at the 20 week anomaly scan), and we were monitored as if the pregnancy was normal, which I loved.
Our son came a day before 40 weeks, though this time my water did not break to kick things off.
My labor with him was fast and furious — by the time we made it to the hospital I was already at 10cm, and he was born vaginally just a couple hours later. 4.5 hours in total!

High-Risk Does not have to mean guaranteed problems
My story is one of a high-risk pregnancy with bicornuate uterus where none of the risks came to light!
Not every high-risk pregnancy will have such smooth sailing, but I hope this post gives you all hope that a high-risk pregnancy with bicornuate uterus is not predestined to be riddled with complications.
Choose a doctor you trust, do your part to live a healthy pregnancy, and do your best to remain positive. You may just have the most typical atypical pregnancy ever!
I am so excited to share with you that I was recently a guest on the podcast “Days with L” where host Lana and I talked about the ins and outs of high-risk pregnancies.
Lana found me through this exact post after she too found out about her bicornuate uterus.
And be sure to head over to Lana’s blog as well! There Lana writes about active women and their wellbeing, and encourages others to pursue happy, healthy lives! Check it out!
Other posts you may like:




wow! cONGRATULATIONS ON THE HEALTHY PREGNANCY & YOUR BABY. KNOWLEDGE IS KEY IN THESE SITUATIONS.
Thank you for posting this! I am 16 weeks with a bicornuate uterus, baby is on my right side. I am due at the beginning of March but am praying to make it to February. You are giving me a little bit of hope!
Congratulations on your pregnancy! I hope you continue to have an un-eventful and full-term pregnancy and smooth delivery! 🙂
Hi Alison, I’m also pregnant currently and my baby is nestled in the left side. Would you be open to chatting with me about your current experience as I am very early, just gone nine weeks.
I hope Alison replies! 🙂 If not, I am happy to talk with you too. You can find me on IG at @ThisIsRealLifeMama
Hi my daughter in law is 12 weeks pregnant & just found out from scan she has bicornuate uterus which was a surprise as she already has a 5 year old girl & carried nearly full term & all they picked up on was that she was small & had to have a lot of growth scans. This is worried me & wish I didn’t go on Google as everything is so negative. She miscarried back in may at 7 weeks but they said it only measured 4 weeks so must of stopped growing weeks before she started bleeding. The only positive I can think of at the moment is she’s already carried a baby & has a little girl so hopefully she can again 🙏
Hello Natalie. I am sending best wishes for an uneventful pregnancy and smooth delivery! It’s possible (and likely) her miscarriage was due to something other than her having a bicornuate uterus. Did you know 1 in 4 pregnancies ends in miscarriage? It’s incredibly common but not spoken about that much. Having bicornuate can present some risk, but that’s also not a guarantee. I hope for exactly like you said, that her body has already proven capable of carrying a baby to term and that she does it again. I hope you get your first grand baby!!
I love how positive this post is. Sometimes when we think something is wrong we tend to worry so much! It isn’t healthy!
Thanks for sharing your experience
Welcome to your beautiful son.
Thank you for sharing!I was high risk with gestational diabetes, and understand having to go to more appointments than normal, and had higher bills because of it. My son was born via a scheduled c section in perfect health, and my blood sugar went right back to normal! Thanks for sharing your story 🙂
What a lovely story. Your fsmily is beAutiful & i am sure this will help others With the same condition know A real life story.
Hot Dang, that was a fast delivery for your son, and really a fairly speedy one for your daughter too! I’m so glad your dreams of being a mother were realized without any major issues!
Interesting! Our bodies are so fascinating.
This is very interesting. I have a tipped uterus, so there was some concern we have issues, but it worked out as well. I am glad to see you have two beautiful kiddos.
This was quite the odyssey but I’m so glad to hear your babies are healthy. You described what was going on clearly but with a minimum of jargon and with an upbeat point of view.
COngrats! I am so glad you were successful!
Wow! So happy for you! Things like that can be hard to overcome, you’re a strong one!
I have never heard of this. thank you for your story.
Thank you for sharing! I’m sure your story will aid in someone elses journey.
I had never heard of this before now. I am so happy for you that you had a healthy little girl. Babies are the best!
What a story! you will be an inspiration to so many others with this same situation!
I love reading pregnancy stories like this! Even when I’m not pregnant.
Congrats on your beautiful children! I can relate to the extra scans, during my last pregnancy, my amniotic fluid became very low, so I had to monitor it all the time to make sure it didn’t become dangerously low. I also had to force myself to slow down and care for myself. Pregnancy can be such a worrying time.
i’VE NEVER HEARD OF THAT CONDITION, SO IT WAS RATHER EYE-OPENING FOR ME. cONGRATS ON YOUR PRECIOUS BABIES & THANKS FOR SHARING, i KNOW IT WILL BE A BLESSING TO SOMEONE WITH THE SAME CONDITION.
I also have a bicornuate uterus an have searched relentlessly through the internet as well to find OTHERS like me. I am in a small town an unfortunately, there is not one person thats similar. I enjoyed reading your post because overall I have had 4 miscarriages. An i am currently pregnant with the fifth. Along with having a rare blood type o-negative. Your story has inspired me not to expect the same thing as I was before which were LOSSes but instead try to not stress and keep positive all because I read your story. Congratulations on your kids!!! Maybe one day it will WORK for me too.
Hi Jessica. I am so sorry that you have experienced four miscarriages. That’s absolutely heartbreaking. I wish you and your growing baby health as your pregnancy progresses. Please keep my updated on how you’re doing!
I am O negative too! Were you able to get pregnant?! :))
Great encouragement for those in similar situations! Congratulations!
Thank you SO much for this post! I have this same condition & only found out during a c section with my first. She was born at 38 weeks and was perfectly healthy minus hip dysplasia that corrected itself within 2 months. As my husband and I try for our second, I have become more nervous now that I KNOW I have this uterus shape. I would be interested to hear from you & other mamas if the risks decreased with each pregnancy or not. Thank you again!
You’re so welcome Athena! I personally felt more at ease trusting in my body, but everybody is different, and I don’t know if medically I was less at risk or not, especially since my second baby was in the other horn! Best wishes!
Wow – i’ve never heard of a bicornuate uterus and cannot believe the story you have to tell. Thank you for sharing this with us!
Im so glad your pregnancies went well. Im silure your stories will encourage others in a high risk category.
What a Wonderful story and an educational post. Im so glad you got to live your Dream and be a mama ????
Thank you so much!
Thanks so much for Sharing your story. Like you, my husband And i learned of my bicornuate Uterus at our 8 week scan this week. I’ve been SCOURING The scary interwebs for more informAtion and So much of it is scary, especially As this is our first child and there are already many unknowns (and it did take us a while to conceive!). Your story brought me great comfort and Some increased optimism.
Hi Liz! I am so glad you found this post and that it gave you comfort. I hope your pregnancy is uneventful and that you have a smooth delivery! Best wishes! Feel free to reach out or email me privately if you want to chat!
Hi,
I am also a mom with bicournaute uterus. My son is now 11 months old. We are really lucky and special mama with special type of uterus. Thanks for sharing your experience.
Hey Revana! Thanks for sharing! I’m so happy to hear another mama with a bicornuate uterus has her little love. Congrats on his upcoming birthday and the anniversary of you becoming a mama!
Hi share your thoughts.. I’m 7 month pregnant .. right corno my baby is in breech position …
Hello. I wish I could help you with medical support, but that is not my realm. Ask your obstetrician any questions and concerns!
Thank you for sharing this story. I found out today I have bicornuate uterus at my 8 week ultrasound. So far all the websites have been pretty scary, so I just refuse to read anything else. I will keep your post as a PREGNANCY goal. Thank you again for sharing positivity, this helps people like me a lot!
Hi Victoria. I’m so glad you found my post, and I wish you a healthy and uneventful pregnancy. Keep me posted on how you’re doing!
Im curious on how much more the costs Added up to. I just found out i have a bic. Uterus and am pregnant. I am afraid of the Potential coSt skyrocketing.
Hi Caroline. Thanks for commenting. Congratulations on your pregnancy! Your costs will depend on your insurance and the doctors you see, so unfortunately I can’t say what your costs will be compared to mine. As far as my experience was, I believe we paid a couple thousand less for my son than for my daughter, but my memory for the specific amount is gone. If cost feels prohibitive to good care, I would speak with your doctors to see how treatment can still be what you need, while limiting more expensive interventions like scans at every appointment. Best of luck!
I would like to share that I am a success story too. I was asked to come in for an ultrasound immediately after I went to an ObGYN saying I was pregnant.
During that appointment I found out I had a Bicorinate uterus and was pregnant with twins. Both on my “Right Half” . I was like let me get this straight, you are telling me I have 2 babies in half the space one baby normally gets in other women?
Wtf? Everything I read was negative and scary so I just stopped reading that type of info and focused back on myself and doing what I needed to do in my immediate reality. Like go to work.
I realize how much discouraging info is out there, so I would just like to share. I carried twins full term a boy and a Girl 37 1/2 weeks…working the whole time until like the last 2-3 weeks with no significant issues. None. My “half a uterus on the right side” stretched out and accomodated my twin pregnancy just fine.
I Only had normal issues like being uncomfortable because I was huge, tired, having heart Burn towards the end etc.
I think much more effort has gone into tragic info sharing in the past and I just want you to know I exist and successfully carried twins. I was 33 when I got pregnant. My twins are 7 years old now and healthy and I am now 40 and reflecting because I dodged the info I received in regards to this issue because I didn’t want to hear it. I am in the middle of having an exceptionally awful period, bleeding amount and pain wise is the reason I found myself here tonight.
God bless you. Your life is what you create. Have faith. I suggest being realistic, but I wasn’t I just ignored the negative things I read and everything went fine. I am not saying every challenge in life is that easy. But this did happen, I am a mom to twins.
Thank you, Kathleen, for sharing your story of success too!! We need to hear more and more about the good experiences so that others can feel hopeful for their journey to motherhood. I am so glad your horn did what it needed to do and then some!!! Amazing that your kiddos are 7 now.
Thanks so much for sharing you’re success stories. I’m 33 right now and have found out I have the same condition. It’s scary knowing I have this and scared also when I looked up online.I’ve had 1 healthy pregnancy cU before and one was misscarried at about 22 wks. I’m hoping for the best but more scared this time around now knowing I have this,but your post on your successful birth stories inspires me and gives me hope,thanks again for your post. So greatful for this blog 🙏
So glad my success stories and the comments of other’s successes give you hope and inspire you!
Thank you for sharing your story. I just found out yesterday I have this condition. I was hoping to have a child soon and became very discouraged. Hearing your story has given me hope.
Hi Anne. I am so glad my story has given you hope! I think learning about it before helped me to be ready for any outcome, versus being surprised with the risks or negative outcomes in the middle of a pregnancy. Best wishes!
This is exactly what I needed. I just discovered I have this at my first 9week scan yesterday. My doctor was so calm and reassuring.. and then I started googling. The internet is far less reassuring so I am so happy to have come across this post! Thank you so much for sharing, I feel like I can breathe again. And reading comments from other women who are in the same boat- it’s just nice to feel like I’m not alone in this.
Hi Leah! I am so glad my post and the other commenters gave you hope. It’s an unnerving thing knowing that there are risks — I am so happy you’re feeling like you can breathe again. I hope you are able to put trust in your body and your doctors, and try to be in the moment. Best wishes!
THANK YOU for sharing. I have the same exact story with our daughter. Left horn, no issues, lots of appointments, full term and vaginal delivery. Now 11 weeks with baby in right horn. Anxiety has started again since I’m unsure of how the right side will handle this, but reading your story helped with my worries. Thank you 🙂
Congratulations to your daughter (and to you!). I hope everything goes smoothly this time around, and the her right horn does what it needs to do!
I have this condition too… I have had 2 miscarriage one at 2 months and one at 4 .. completely lost on what to do ahead …try naturally or go for surgery …. I personally have lost hopes… But reading your story feels good
Oh my gosh! I am so so sorry that you lost your babies. It’s so hard to hang onto hope when your experience has included losses! I hope you can find a specialist who can help identify the best steps forward for you!
I have a bicornate uterus as well. My baby is on the left side. I’ve had a lot of pain on the left side and my doctor thinks it’s round ligament pain. Did you have any pain or discomfort as well? I am at a loss as to what is normal and what isn’t. Thank you!
Hi Briana. Congrats on your pregnancy! I am sorry you’re having pain!! I did not have any round ligament pain. The range of what’s normal is so broad, both in typical and high risk pregnancies, so I think the best thing to do is speak with your doctor and seek a specialist if you don’t feel they are educated enough in bicornuate uteri. I felt so comfortable with my perinatal specialists, especially my first pregnancy, because I felt like they understood bicornuate inside and out. Besides your medical care, I want you to pay special attention to your mental health. High risk adds so many layers of stress and it’s easy to feel like something could go wrong at any moment. Some women find mantras really helpful such as “I can trust my body” or “My body and my baby are working together”, etc. I hope everything goes smoothly for a full-term delivery!
Wow! This gave me so much calmness. I am experiencing my first pregnancy & I just found out at my first ultrasound that I have this condition. As I am one of those who tend to recur to google for answers. Even after they said I shouldn’t have anything worry about. 😖
But it brings me great peace knowing I too shouldn’t stress or worry.
Thank you so much for sharing your story! Be blessed always!
Congratulations on your first pregnancy! I am so pleased my post brings you peace! I hope your pregnancy is uneventful and lovely. Best wishes!
Thank you thank you thank you for sharing this. I’ve had three miscarriages and found out today I have a heart shaped uterus. I’m not sure how extreme it is but your story totally gives me hope for the future ❤️
Gosh, Annabel, I am so sorry you have had to go through miscarrying three times. Sending you so much love and strength. I hope with this new information that your doctors are able to provide support to help you going forward. My thoughts are with you!
So grateful that you shared your success story. I have also been riddled with anxiety and fear about what will happen to baby because of my bicornuate uterus. It feels like everything on the internet just keeps pointing to gloom and doom, but once I started looking for the light I found your story. Whatever happens, I think just that added hope provides a sense calm and also knowing that others have been through the same. We got this mothers!
Hi Kaylee! You’re so right that so much online is scary to read and absolutely produces even more anxiety!! I am so glad you found my post and I hope you continue to remember it when you feel worried. Best wishes!!
I needed this today. I just found out today I have a heart shaped uterus. I had a miscarriage (my first pregnancy) in October and decided to switch to a different dr because I just felt like something was not right and was not given the care I needed during that emotional time. My message is to be an advocate for your health! If you are feeling like your health is not getting taken care of switch to a different dr. As much as it sucks that there are women like me dealing with this, it’s calming to find articles like this and to see you are not alone. Surround yourself with supportive family, friends, a great dr, and never lose faith in God. Thank you for sharing your story. It gives me hope.
Hi Paige. I am so sorry that you had a miscarriage and that you didn’t receive the medical support and care you needed. I am glad that my post was helpful for you today and I wish you the best with your future fertility journey. I love your message and the meaning you’ve given to your experience. Sending love!
I’m pregnant very early stages and I’m due august 2022. This is just what I needed to hear after finding out my baby is nestled in the left side. I’d love to connect with people currently going through the same to share experiences and understand the risks.
Hi Lauren, congratulations on your pregnancy! I’m so glad my post was helpful in offering you hope! This Fb group is a great community of other ladies with bicornuate uteri and I think you’ll find it helpful too: https://www.facebook.com/groups/153557255241412/ Best wishes!
Hi, reading this brought tears to my eyes and I didn’t feel so alone after reading the comments. I was just told of this a few days ago, after I had to advocate for an ultrasound. I’m definitely in a place of fear as I am trying to conceive. This page is what I needed today, thank you.
Hi Vanessa,
I’m so glad my story, and all the comments related to it, helped you not feel so alone. I’m so proud of you that you advocated for yourself and got an ultrasound. I wish you the smoothest and most uneventful journey to motherhood possible!
Love, Christina
Iam diagnosed bi cornuate uterus 29th week pregnancy today iam go for the scan in that iam getting some difference in fetal biometry in weeks.it is any risk in my condition please tell me mam
Hello. Congratulations on you pregnancy! I wish I were able to answer your question, however I am just a person with my own bicornuate story and not an obstetrician. Best to ask your providers. I will be hoping for the best for you!
I just stumbled upon your story and I’m glad I did! I also have a bicornuate uterus and am currently 10 weeks pregnant with my first pregnancy that has gone this far (we struggled to conceive and had one early miscarriage). I didn’t know i was bicornuate until after we had been trying for over a year. I just saw my high-risk OB for the first time yesterday and he was encouraging and optimistic, but your story is so encouraging to hear as well! So thank you for sharing! My baby is in my right horn and so far things are looking great, praise God!
Hi April. Congrats on your pregnancy! I am about six weeks ahead with my third baby now! I am so sorry you struggled to conceive and had a miscarriage. Even if it’s early, it’s still so heartbreaking. I hope your pregnancy continues smoothly and uneventfully!
Hello!))
Several years back, I had went to the doc and found out I had bicornuate uterus and possibly have PCOS too.
My periods skip a lot and if I bleed I bleed 7 days straight. My husband and I have been trying to get pregnant for two years now and I can’t seem to conceive. Now I am on day 100 since my last period (negative pregnancy test) It is all frustrating because I can’t seem to find a obgyn that understands what my issues are other than just pushing birth control pills or doing ivf.
What are some things that you have done or recommend?
what are symptoms of your pregnancy? how soon did you know?
Hi Valya. Oh my gosh that is so frustrating! I am sorry your OB hasn’t been any help. I would recommend you find a perinatal specialist in your area — they are well versed in perinatal conditions including bicornuate uteri! My guess with your periods often skipping, would be that you are not ovulating, so my other recommendation to you is to track your cycles using FAM (Fertility Awareness Method) which involves taking your basal body temperature every day before you get out of bed, and noting your cervical fluid which changes at different points in the cycle. Best of luck!
Wow, thank you for this. I am guilty of being deep in the rabbit hole since I just experienced a missed miscarriage and found out today I have a bicornuate uterus. This blog gives me hope since the internet is scary.
Hi Janvika, thanks for your message. I am so sorry about your missed miscarriage. That is heartbreaking. I am so glad my post was able to give you hope. I wish you the best!
Thank you for sharing this, I miscarried this past October (7 weeks) and we later got confirmation that I have a Bicornuate uterus. It definitely gives a defeating feeling.. especially with this being my first pregnancy. We’re eager and nervous to try again, but just hope and pray for a successful pregnancy journey and smooth delivery. It’s exhausting going through this, I just turned 30 so I feel rushed, but am ready to try again God willing. Hang in there my fellow Biconuate gals, we’re going to be okay!